Plantar Fasciitis Embolization (PFE) TreatmentMinimally Invasive Foot Pain Relief Kansas City
What is Plantar Fasciitis
Plantar fasciitis occurs when the plantar fascia—the band of tissue connecting the heel bone to the toes—becomes inflamed or damaged due to stress or overuse.
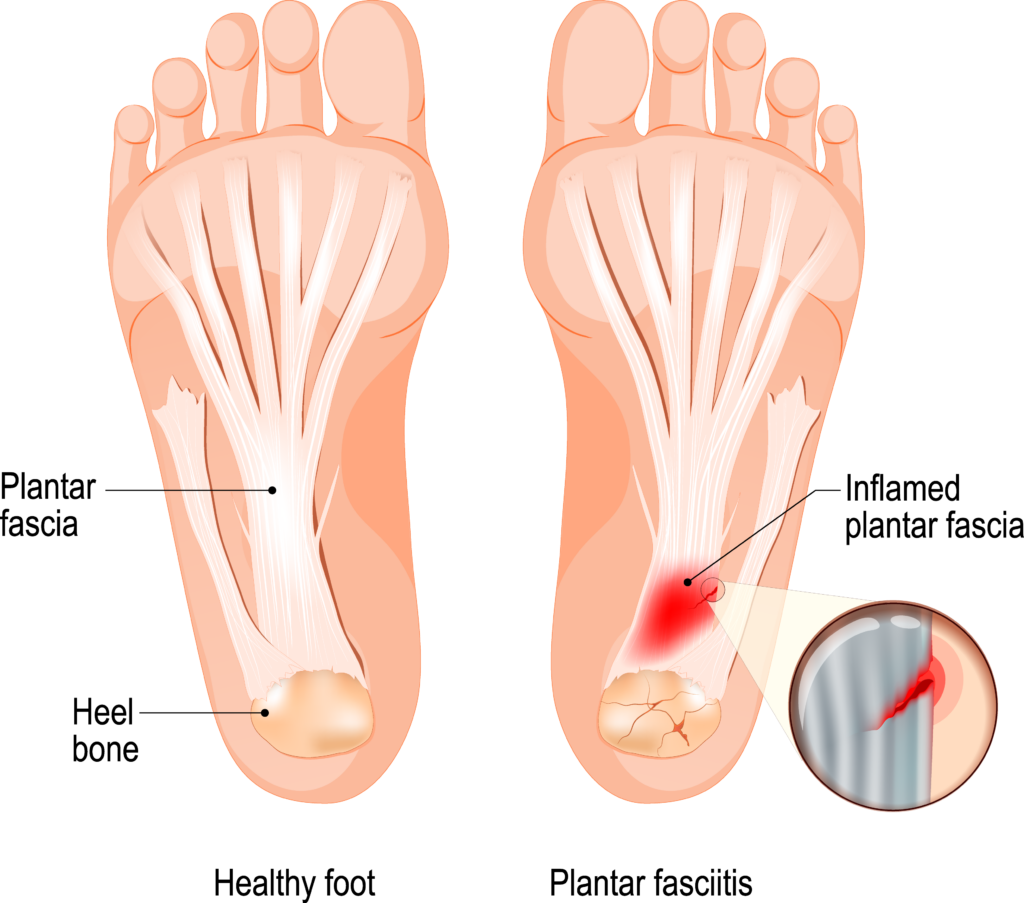
What Are the Symptoms of Plantar Fasciitis?
If left untreated, the following symptoms may be present:
- Worsening heel pain
- Development of bone spurs
- Rupture of the plantar fascia
Risk Factors of Plantar Fasciitis
Age
Common in individuals aged 40–60.
Obesity
Increased stress on the plantar fascia.
Prolonged Standing
Common among workers on their feet all day.
Foot Structure
Flat feet or high arches.
What is Plantar Fasciitis Embolization (PFE)?
PFE is a state-of-the-art minimally invasive procedure performed by board-certified interventional radiologists. This outpatient treatment targets the root cause of pain and inflammation.
How is PFE Performed?
1
A tiny catheter (thinner than a spaghetti noodle) is inserted through a small pinhole in the leg.
2
Blood vessels feeding the inflamed plantar fascia are identified.
3
Microscopic particles are injected to block abnormal blood flow, reducing inflammation and pain.
4
Closure: The instruments are removed, and a pressure dressing is applied.
Why Choose PFE?
Minimally Invasive
No incisions or stitches required.
Faster-relief
Results often appear quicker than traditional treatments.
Long-lasting outcomes
Many patients experience significant, prolonged pain relief.
Conservative Treatments for Plantar Fasciitis
Before PFE, many patients try the following options:
Corticosteroid Injections
- Effective for short-term relief (up to 3 months).
- Repeated use may cause reduced efficacy and increased risks.
Physical Therapy and Exercises
- Stretching routines targeting the plantar fascia and Achilles tendon.
- Ice therapy and deep tissue massage for pain relief.
- Many patients achieve success, but some require additional treatments.
Medications
- Over-the-counter NSAIDs help reduce pain and inflammation.
- Long-term use can lead to serious side effects.
Bracing and Assistive Devices
- Arch supports or custom orthotics.
- Night splints to maintain foot alignment.
Other Minimally Invasive Treatments
- Extracorporeal Shock Wave Therapy (ESWT): Uses sound waves to promote healing.
- Platelet-Rich Plasma (PRP) Injections: May provide temporary relief.
- Dry Needling: Stimulates healing and increases blood flow.
Surgery
- Surgery is a last resort after 6–12 months of failed conservative treatments.
- Risks include scarring, plantar fascia rupture, and prolonged recovery.
Frequently Asked Questions about Plantar Fasciitis Embolization
Who is a candidate for PFE?
- Anybody with pain due to plantar fasciitis that has lasted more than 3 months
despite conservative treatment, especially if there is still pain after a different
minimally invasive therapy. - Patients who have complete plantar fascia rupture are not candidates.
Am I awake for the procedure? Is there any pain?
- You will get IV twilight sedation to help you relax and not feel pain.
- You get a small numbing injection (like at the dentist) before the doctor enters the artery. This can sting for a few seconds.
- You may feel your normal Achilles pain when the doctor is injecting dye and medicine.
How is the procedure performed?
- The artery going into the leg will be accessed safely with a needle using ultrasound. The needle will then be replaced by a small tube.
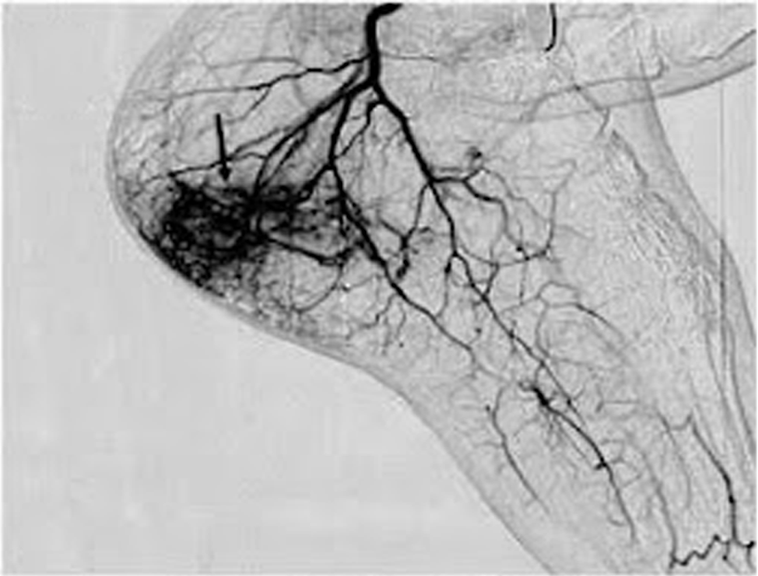
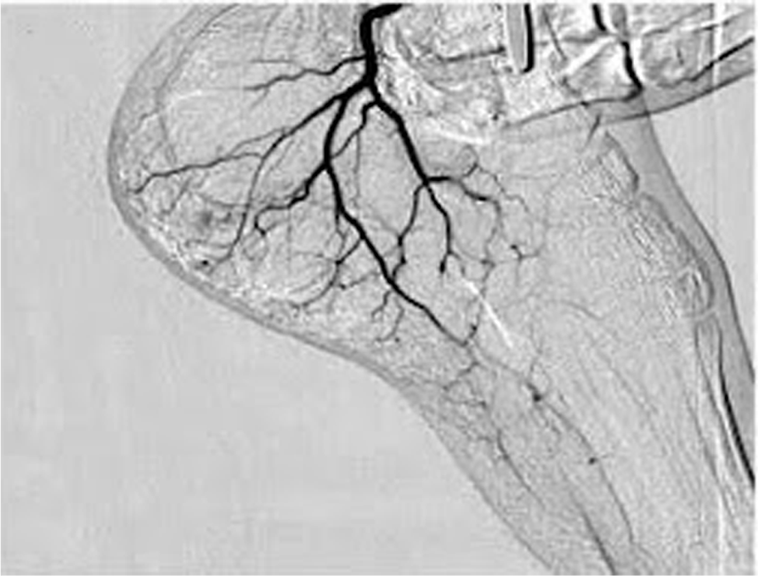
- The doctor will then inject x-ray dye down the leg to take an angiogram (blood vessel picture) of your foot and ankle.
- Your doctor will use the picture as a map to place even tinier catheters into the artery branches supplying the inflammation.
- The doctor will then remove everything and hold pressure to close the pinhole in your artery. You will go home with just a small 1 inch bandage.
What are the risks of PFE?
- There is a very small risk of bleeding where the doctor went into the artery.
- There is an extremely small risk of infection.
- The arteries to the plantar fascia often send tiny branches to your skin. Blocking them can cause a small rash. This is not painful and resolves within 2 weeks.
What are my restrictions after the procedure?
- You must lie flat with your leg straight for 1-2 hours after the procedure.
- You can take the dressing off and shower the next day.
- You should hold pressure on your groin while coughing, sneezing, or straining in the bathroom.
- You cannot perform strenuous activity or lift the weight of more than a gallon of milk for 1 week after the procedure.
- Normal walking and light activity are not restricted.
- You can drive the next day if you received IV sedation.
When will the pain get better? How long does the pain relief last?
- There may be a few days of worsening pain and stiffness. This feeling will go away, leaving real pain relief.
- More than 80% of people experience long-lasting pain relief.
- Patients should continue their stretching and strengthening exercises to prevent the pain from coming back.
- If the pain comes back, repeat PFE or another treatment can be considered.
Take the First Step Toward Pain Relief
At Vascular & Interventional Specialists of Kansas City, we are committed to providing innovative, minimally invasive treatments to help you live pain-free.
Contact us today or call (816) 720-5332 to schedule your consultation. Let us help you take the next step toward recovery.
If you experience emergency symptoms, such as severe pain or difficulty moving, call 911 immediately.
