Pelvic Venous Disease Treatment Kansas City
(Pelvic Congestion Syndrome) Minimally Invasive Gonadal Vein Embolization
What is Pelvic Venous Disease?
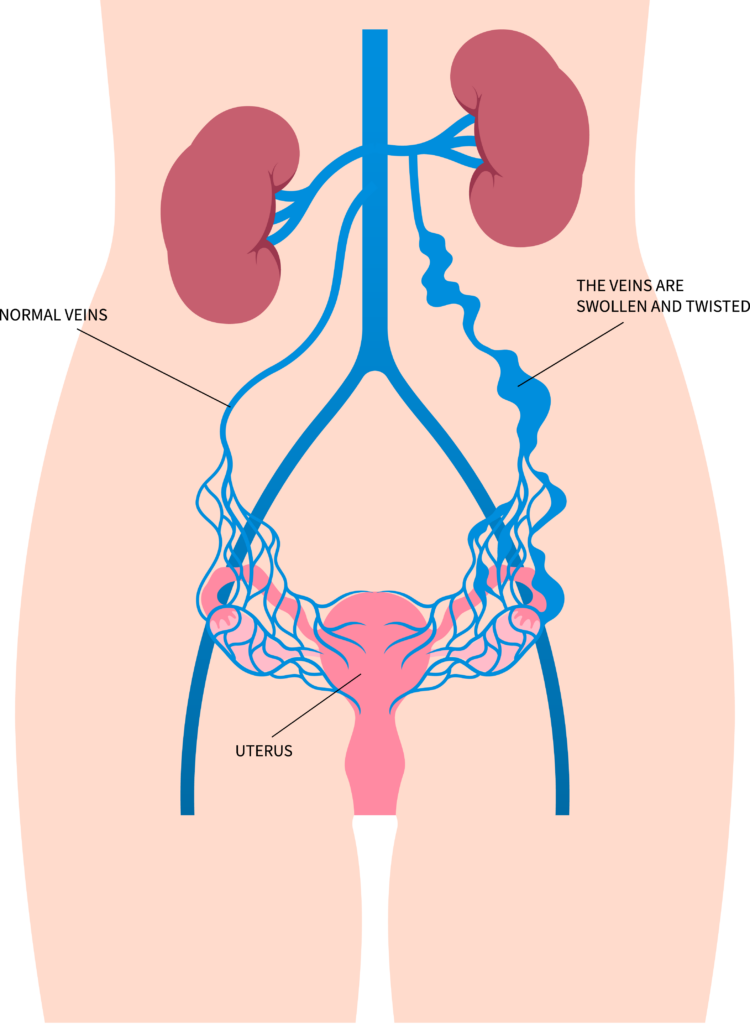
Pelvic Venous Disease, formerly known as Pelvic Congestion Syndrome (PCS, is a condition caused by varicose veins in the pelvic region, leading to chronic pelvic pain. These veins become enlarged and allow blood to pool, causing pressure and discomfort. PVD primarily affects reproductive age women and is often underdiagnosed.
What Are the Symptoms of Pelvic Venous Disease?
Common symptoms of PVD include:
- Chronic pelvic pain, often described as dull or aching, lasting more than 6 months.
- Pain that worsens with prolonged standing, sitting, or physical activity.
- Heaviness or pressure in the pelvic region.
- Visible varicose veins on the thighs, buttocks, or vaginal area.
- Pain during or after intercourse.
- Worsening symptoms before menstruation.
Risk Factors of Pelvic Venous Disease
Multiple pregnancies
Increased blood flow and hormonal changes can weaken vein walls.
Family history
Family history of varicose veins or venous disorders.
Hormonal changes
Elevated estrogen levels can contribute to vein dilation.
Prolonged sitting or standing
Poor circulation exacerbates venous issues.
What is Gonadal Vein Embolization for PVD?
A Gonadal Vein Embolization is a minimally invasive procedure used to diagnose and treat Pelvic Venous Disease. This advanced technique helps relieve pain by targeting and closing the problematic veins that cause PVD.
How It Works:
A venogram (a specialized X-ray) is performed to identify the affected veins.
Using a catheter, the doctor delivers treatments to block or close the problematic veins, restoring proper blood flow.
How is Venogram with Intervention Performed?
1
Venous Access: A small needle is used to access a vein in the neck, arm, or groin.
2
Venogram Imaging: X-ray dye is injected to visualize the veins in the pelvic area.
3
Targeted Intervention: A catheter is guided to the affected veins, where embolization or sclerotherapy is performed.
4
Closure and Recovery: The catheter is removed, and the access site is closed with a small bandage.
Why Choose Venogram with Intervention for PVD
Minimally Invasive
No incisions or stitches required.
Quick recovery
Most patients return to normal activities within a few days.
Effective pain relief
Targets the root cause of PVD by treating problematic veins.
Outpatient procedure
Performed in a single visit, avoiding the need for major surgery.
Conservative Treatments for Pelvic Venous Disease
Before considering a venogram with intervention, patients may explore these non-invasive options
Compression garments
Specialized pelvic or abdominal compression may improve symptoms.
Pain management
Over-the-counter NSAIDs can provide temporary relief.
Exercise
Regular physical activity promotes healthy blood flow.
Lifestyle changes
Avoid prolonged sitting or standing to improve circulation.
Frequently Asked Questions about Venogram for PVD
Is the procedure painful?
The procedure is performed under local anesthesia with sedation, and most patients report little to no discomfort.
How long does the procedure take?
The procedure typically takes 1–2 hours, depending on the severity of the condition.
When will I feel relief?
Most patients experience significant symptom relief within days to weeks after the procedure.
Are there risks involved?
Risks are minimal and may include minor bleeding or infection at the access site. Your doctor will discuss any potential complications.
Can the condition return after treatment?
While treatment is highly effective, ongoing lifestyle changes and follow-up care are recommended to prevent recurrence.
Is this procedure covered by insurance?
Many insurance plans cover venogram with intervention if deemed medically necessary. Check with your provider for details.
Take the First Step Toward Pain Relief
At Vascular & Interventional Specialists of Kansas City, we are committed to providing innovative, minimally invasive treatments to help you live pain-free.
Contact us today or call (816) 720-5332 to schedule your consultation and take control of your vascular health.
If you experience emergency symptoms, such as severe pelvic pain or shortness of breath, call 911 immediately.
